Struggling with your breathing is a pressing concern and one that might be your reason for calling us at Physit.
Our Physiotherapists regularly review medical journals for any updates to research. Take a look at one of our recent presentations regarding physical strength and the relationship to your respiratory system!
For any further regarding setting up an initial consultation or our services and prices please contact our Admin team on 07714 244 438 or email us on info@physit.co.uk.
What happens during breathing?
During breathing there are two distinct phases, inspiration (inhalation) and expiration (exhalation).
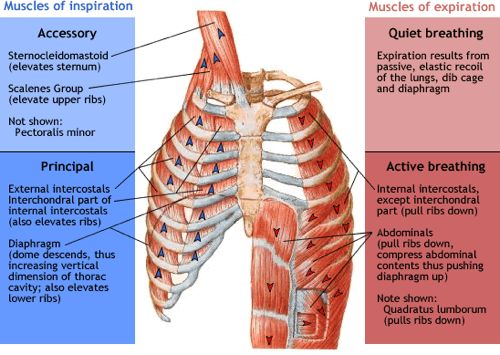
Inspiration: During inspiration, the anterior-posterior, vertical, and transverse dimensions of the thorax increase through the contraction of our muscles.
The contraction of the diaphragm causes its central tendon to be pulled inferiority which flattens the diaphragm and increases the vertical dimensions of the thorax (Shahid and Burns, 2020).
Muscles between the ribs called the external intercostal contract raising the lateral part of the ribs which causes a bucket handle motion to increase the transverse diameter of the thorax while vertebrosternal (true) ribs follow this pump handle motion which raises the sternum and increases the anterior-posterior dimensions of the thorax (Donley and Loyd, 2020).
The serratus posterior superior attaches to ribs 2 through 5 and help elevate the rib during inspiration while the scalenes can help to elevate the first and second ribs when the neck is fixed. In forced inspiration and when needed the pectoralis minor assists in lifting third, fourth and fifth ribs.
Expiration: During expiration, the diaphragm relaxes while the abdominal muscles and other accessory muscles [quadratus lumborum (QL), latissimus dorsi (lats) and serratus posterior inferior] contract.
The contraction of the abdominal muscles along with the internal intercostals compresses the lower part of the thorax and increases intra-abdominal pressure while the QL’s fix the 12th ribs and the lats and serratus posterior inferior help to depress the ribs.
The serratus posterior inferior helps depress the ribs through their attachment to the vertebrae and ribs 8 through 12 (Donley and Loyd, 2020). This depression of the thorax decreases its volume and increases the pressure, causing the lungs to contract and forcing the air out.
How is this relevant to spinal mobility and core strength?

The interaction of the thoracic spine(Tsp) and ribs is important when looking at a persons ability to achieve a good chest expansion and therefore their ability to inflate and deflate their lungs effectively.
The ribs attach onto the thoracic spine at the back and the sternum at the front. If the thoracic spine loses range of movement (ROM) then this loss of ROM will affect how the ribs interact with the spine and affect the ribs ROM. A loss of Tsp ROM and ribs can affect a persons ability to fully expand their thorax which can in turn adversely affect their breathing.
Chest expansion, respiratory function, and thoracic vertebral pain are adversely affected by a reduction in the mobility of the thoracic vertebrae and changes in the thoracic and lumber angles (Wirth et al., 2014).
There is evidence to show that an increase in the kyphosis of the Tsp can lead to a decrease in lung function in women however the study did not show the same decrease of lung function in men.
This may be due to the smaller number of participants or possibly the fact that men carry more muscle mass and therefore are able to use their accessory breathing musculature to help them breath better despite the increased Tsp kyphosis (KYPHOSIS PROGRESSION AND PHYSICAL FUNCTION IN WOMEN AND MEN: THE FRAMINGHAM KYPHOSIS STUDY, 2015).
Therefore doing spinal mobility exercises can keep the Tsp moving more effectively and strengthening can stabilise the spine and limit your chances of getting an increased Tsp kyphosis which can lead to a decrease in your lung function.
A study by Jung and Moon, 2015 showed that self Tsp mobilisation has the ability to improve a persons chest expansion but not lung function. The lack of improvement in their lung function may be due to the fact that the participants were younger, healthy individuals.
There are studies showing that spinal mobilisation exercises and core strengthening can improve respiratory function in stroke patients and those with COPD.
References:
Donley, E. and Loyd, J., 2020. Anatomy, Thorax, Wall Movements. [online] Ncbi.nlm.nih.gov. Available at: <https://www.ncbi.nlm.nih.gov/books/NBK526023/> [Accessed 18 May 2020].
Jung, J. and Moon, D., 2015. The effect of thoracic region self-mobilization on chest expansion and pulmonary function. Journal of Physical Therapy Science, 27(9), pp.2779-2781.
Lorbergs, A., Murabito, J., Jarraya, M., Guermazi, A., Allaire, B., Yang, L., Kiel, D., Cupples, L., Bouxsein, M., Travison, T. and Samelson, E., 2017. Thoracic Kyphosis and Physical Function: The Framingham Study. Journal of the American Geriatrics Society, 65(10), pp.2257-2264.
Park, S., Kim, S. and Min, K., 2017. The immediate effects of rib cage joint mobilization and chest wall stretch on muscle tone and stiffness of respiratory muscles and chest expansion ability in patients with chronic stroke. Journal of Physical Therapy Science, 29(11), pp.1960-1963.
Physiopedia. 2020. 949 937 Muscles-Of-Respiration.Jpg. [online] Available at: <https://www.physio-pedia.com/File:949_937_muscles-of-respiration.jpg> [Accessed 27 May 2020].
Shahid, Z. and Burns, B., 2020. Anatomy, Abdomen And Pelvis, Diaphragm. [online] Ncbi.nlm.nih.gov. Available at: <https://www.ncbi.nlm.nih.gov/books/NBK470191/> [Accessed 18 May 2020].
The Gerontologist, 2015. KYPHOSIS PROGRESSION AND PHYSICAL FUNCTION IN WOMEN AND MEN: THE FRAMINGHAM KYPHOSIS STUDY. 55(Suppl_2), pp.361-361.
Wirth, B., Amstalden, M., Perk, M., Boutellier, U. and Humphreys, B., 2014. Respiratory dysfunction in patients with chronic neck pain – Influence of thoracic spine and chest mobility. Manual Therapy, 19(5), pp.440-444.
Yilmaz Yelvar, G., Cirak, Y., Parlak Demir, Y., Dalkilinc, M. and Bozkurt, B., 2016. Immediate effect of manual therapy on respiratory functions and inspiratory muscle strength in patients with COPD. International Journal of Chronic Obstructive Pulmonary Disease, p.1353.





